IBS & TCM
Irritable bowel syndrome (IBS) is a functional gastrointestinal disorder of the large intestine characterized by symptoms of abdominal pain or cramping, changes in bowel movements including diarrhea, constipation (or both alternating), bloating, gas, and whitish mucus in the stools. Traditional Chinese Medicine can be a solution for many suffering from IBS.
IBS BIOMED OVERVIEW
IBS is a disorder of the enteric nervous system, one of the main divisions of the autonomic nervous system. It governs the function of gastrointestinal tract including muscle contractions in the bowel, ion secretion and absorption, and gastrointestinal blood flow. From a biomed standpoint, there are three different forms of IBS consisting of diarrhea-predominant (D-IBS), constipation-predominant (C-IBS), and alternating constipation and diarrhea (A-IBS). Finally, we will address the TCM patterns later in this article.
Causes of IBS
The cause of IBS is not fully understood. However, researchers believe there are many factors that can contribute to the development of the condition. These include stress, depression, anxiety, bacterial infections in the digestive tract, small intestinal bacterial overgrowth (SIBO), food intolerances or sensitivities, and medications.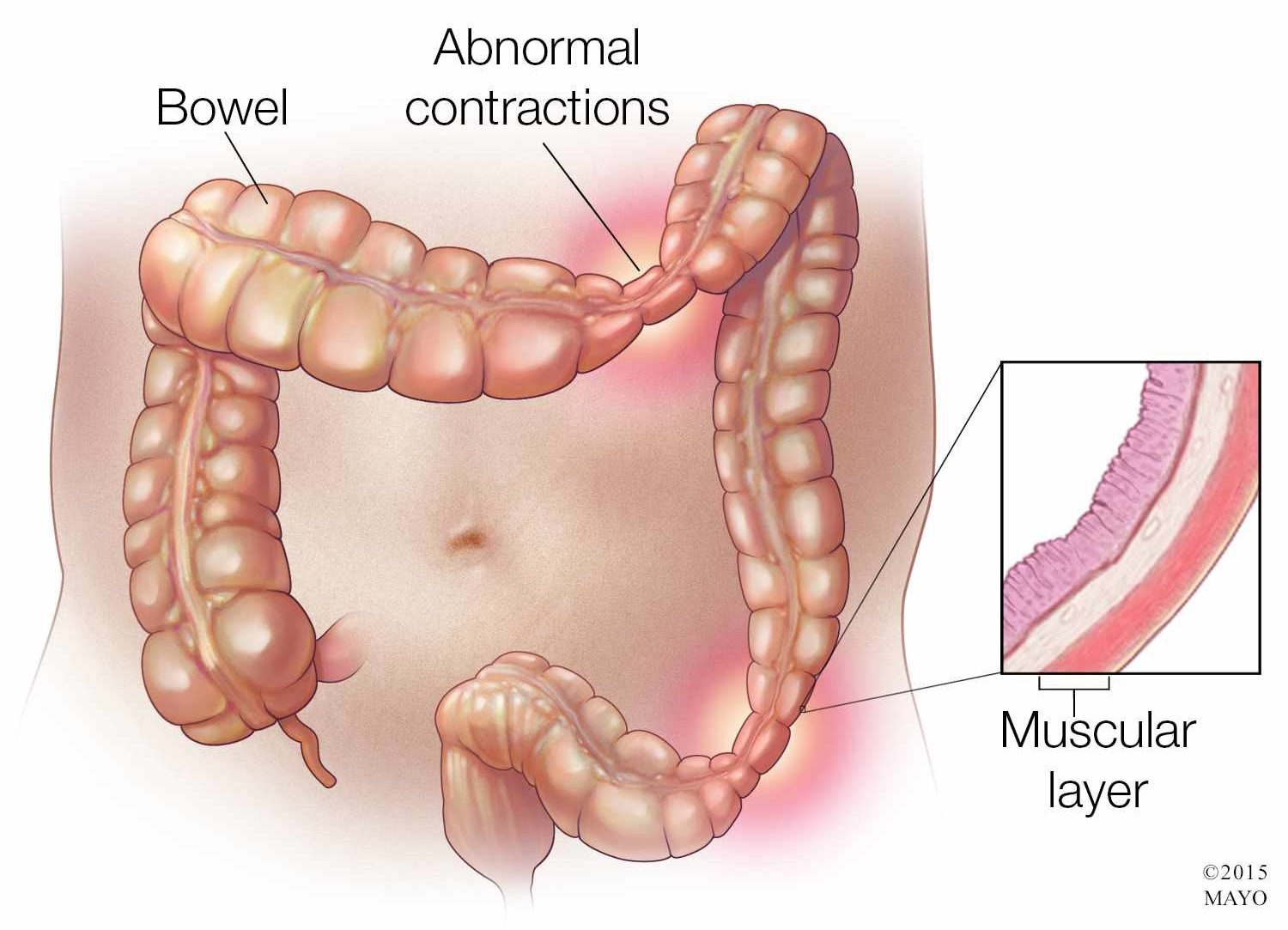
In both animal and human studies, stress is a trigger for IBS. The stress can be anything that stimulates the GI tract including mental/emotional stress, physical stress, or diet changes. In IBS patients, there is also an increased response of the enteric nerve to these stressors. Visceral hypersensitivity is a character trait in IBS patients which amplifies sensory signals that come from the gut at brain and spinal cord level. The nerve pathways in the GI tract become sensitized to stimulation, resulting in over-reactivity and pain amplification.
Compromised Liver Function
Such hypersensitivity may be linked to hepatic (Liver) injury and metabolic syndromes. Thus, a poorly functioning liver is unable to remove toxins from the blood (this is consistent with TCM theory and practice). Thus, when the toxins build up in the blood, they can affect the function of the nervous systems. The liver is an important organ that participates in lipid metabolism and helps to maintain the structure of the nervous system. Reduced liver function can affect the repair of the entire nervous system. This causes the hypersensitivity of the enteric nervous system as well as the brain and spinal cord.
Bacterial Infections
Also, bacterial infections of the GI tract or SIBO is another major IBS causing factor. A statistical study showed that among the examined IBS patients, 84% of them had SIBO. 66% of children diagnosed with IBS have SIBO. In SIBO or bacterial infections of the GI tract, the microbiome balance can become altered. Intestinal pathogenic or unfriendly bacterium and bacterial toxins can affect the enteric neural function leading to disruptions in the coordinated rhythm of the intestinal muscles that contract and relax as food moves through.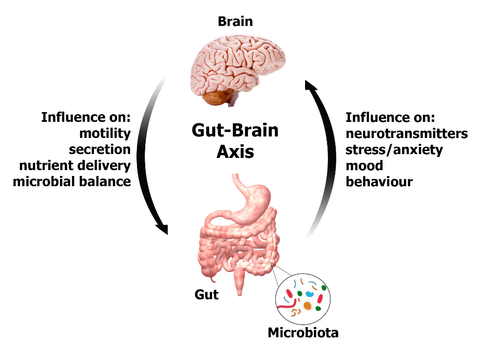
Although there are three main biomedicine forms of IBS, there is also post-infectious IBS (PI-IBS) which results after a case of gastroenteritis. There are many studies that show a similarity between PI-IBS and D-IBS (remember D = Diarrhea). A study of patients with D-IBS and PI-IBS found that the fecal microbiota differed greatly between healthy controls and IBS patients. Microbial dysbiosis of D-IBS and PI-IBS patients did not differ, leading to the conclusion that these conditions may share a similar pathophysiology. Also, a study with rodent models with PI-IBS in which after being given probiotics showed modulation in visceral hypersensitivity and muscle hyper-contractibility. This suggests that the GI microbiota can influence the development of IBS.
Food Allergies
Additionally, nutrient hypersensitivity may also be one of the causes of IBS. Food sensitivities typically come on due to an altered epithelial permeability, otherwise known as leaky gut. Multiple studies have shown increased levels of both small and large intestine permeability in IBS patient regardless of the sub-type. Leaky gut allows an increased antigen load to enter through the intestinal epithelium. Underneath the intestinal epithelium, there are a variety of immune cells, including B cells, T cells, neutrophils and dendritic cells which are antigen-presenting cells.
Binding of the antigens with dendritic cells results in the activation of B lymphocytes to produce IgE/IgG antibodies and cytokines. Also, acute stress can increase the release of mast cells and eosinophil activation which also leads to the release of multiple chemical mediators. Together, these pathways may lead to altered gut function, minor inflammation or autoimmunity, and abnormal mucosal sensitivity. Leaky gut also allows bacteria and viruses to pass through the epithelium. Consequently, this can irritate the enteric nerves causing abnormal smooth muscle contraction leading to chronic diarrhea or constipation.
IBS & TCM
Traditional Chinese Medicine (TCM) and functional medicine can offer safe, effective, natural and drug-free way to address IBS. Thus, this holistic healthcare system looks at the body differently than biomedicine. Likewise, according to Chinese Medicine the body is like a garden that we cultivate and maintain in order to remain strong and grow healthy. Good health occurs when all the organs and systems are balanced and working together.
HOW DOES YOUR GARDEN GROW?
According to Chinese medical models, there are several possible causes for IBS.
Role of the Spleen
One them is an imbalance of the Spleen. In TCM, the Spleen is the organ in charge of digestion and assimilation of foods and liquids. One of the main functions of the Spleen is to aid in the production of Spleen Qi. Spleen Qi is the energy that provides proper and nourishment to the entire body.
Finally, another function of the Spleen is to produce blood from the food it breaks down and to convert it into usable energy to power your body. If the Spleen isn’t properly working, the body’s energy levels will occur and illness may develop.
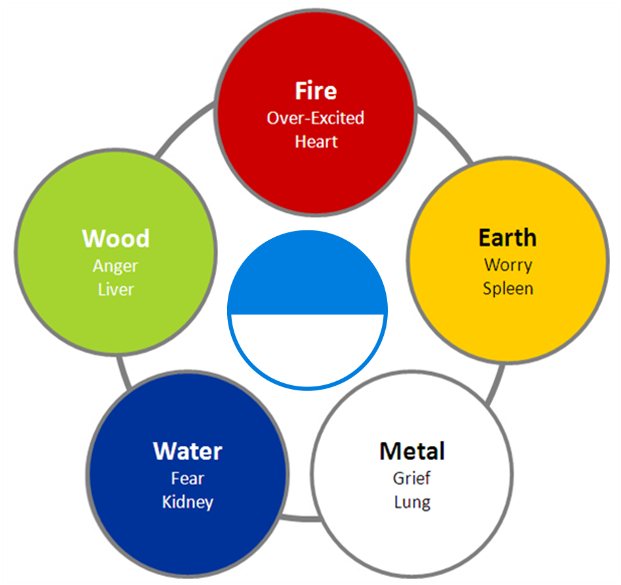
Consequently, the Spleen is easily affected and weakened by poor eating habits, and diet, antibiotics, excessive worry, or a weak constitution. So, when a weakened Spleen cannot metabolize or process food efficiently, “dampness” appears in the body. Dampness occurs when rotting, undirected food sits in the gut, causing a variety of symptoms. Hence, if dampness rises to your head, you may experience headaches, a foggy feeling and an inability to concentrate. Over time, dampness can lead to bloating, fullness and loose stools.
Role of the Liver
Another possible cause is an imbalance in the Liver. According to Chinese medicine, the Liver is associated with emotional health. Stress, frustration and anger directly influence the function of the Liver.
Additionally, alcohol, drugs and medications, or a poor diet can further compromise the function of the Liver. When this happens, Liver energy overflows, in a figurative sense, and attacks the Spleen. If the Spleen is already weakened, it can be easily overcome. The result can be stress-induced IBS.
Eventually, if the Liver is compromised, one may experience alternating diarrhea and constipation, as well as bloating, gas, headaches, and dull pain. In this case, the Liver may be the root of the problem, and the Spleen the secondary cause.
Role of the Kidney
An imbalance in Kidney Yang can also cause IBS symptoms. Kidney Yang is energy that provides warmth for the body. This energy warms up the Spleen to aid in the digestion and breakdown of food. If Kidney energy is compromised, early morning diarrhea, bladder incontinence, cold limbs, impotence, a sore back and weak knees might occur.
In this context, TCM can create a clear picture of the root imbalances that lead to IBS symptoms. When you meet with us we determine what organ and systems are contributing to IBS symptoms. We may suggest adjunct therapies such as TCM formulas, supplements, dietary changes, breathing techniques, mindful movement, stress reduction techniques, etc in order to maximize healing.
In conclusion, TCM and Functional Medicine can provide safe, natural, drug free and effective ways to treat IBS. Give me a call for a free 15 min to see if I can help you or someone you know for IBS and other GI issues!
References
- Chey, William D., Jacob Kurlander, and Shanti Eswaran. 2015. “Irritable Bowel Syndrome: A Clinical Review.” JAMA: The Journal of the American Medical Association 313 (9): 949–58.
- Li, Dan-Yan, Yun-Kai Dai, Yun-Zhan Zhang, Meng-Xin Huang, Ru-Liu Li, Jia Ou-Yang, Wei-Jing Chen, and Ling Hu. 2017. “Systematic Review and Meta-Analysis of Traditional Chinese Medicine in the Treatment of Constipation-Predominant Irritable Bowel Syndrome.” PloS One 12 (12): e0189491.
- Li, Lei, Herong Cui, Tong Li, Jinchai Qi, Hongshan Chen, Feng Gao, Xuehao Tian, et al. 2020. “Synergistic Effect of Berberine-Based Chinese Medicine Assembled Nanostructures on Diarrhea-Predominant Irritable Bowel Syndrome In Vivo.” Frontiers in Pharmacology 11 (August): 1210.
- Xiao, Hai-Tao, Linda Zhong, Siu-Wai Tsang, Ze-Si Lin, and Zhao-Xiang Bian. 2015. “Traditional Chinese Medicine Formulas for Irritable Bowel Syndrome: From Ancient Wisdoms to Scientific Understandings.” The American Journal of Chinese Medicine 43 (1): 1–23.
- Yan, Jing, Zhi-Wei Miao, Jun Lu, Fei Ge, Li-Hua Yu, Wen-Bin Shang, Li-Na Liu, and Zhi-Guang Sun. 2019. “Acupuncture plus Chinese Herbal Medicine for Irritable Bowel Syndrome with Diarrhea: A Systematic Review and Meta-Analysis.” Evidence-Based Complementary and Alternative Medicine: eCAM 2019 (April): 7680963.
- Zhu, Jia-Jie, Shan Liu, Xiao-Lan Su, Zi-Song Wang, Yu Guo, Yi-Jie Li, Yang Yang, et al. 2016. “Efficacy of Chinese Herbal Medicine for Diarrhea-Predominant Irritable Bowel Syndrome: A Meta-Analysis of Randomized, Double-Blind, Placebo-Controlled Trials.” Evidence-Based Complementary and Alternative Medicine: eCAM 2016 (July): 4071260.
- Merck Manual / Wei Labs

